French Toast With Minimal Effort
I love a good breakfast casserole that can be prepped ahead of time. This Brioche French Toast Casserole is absolutely perfect for an occasion like...
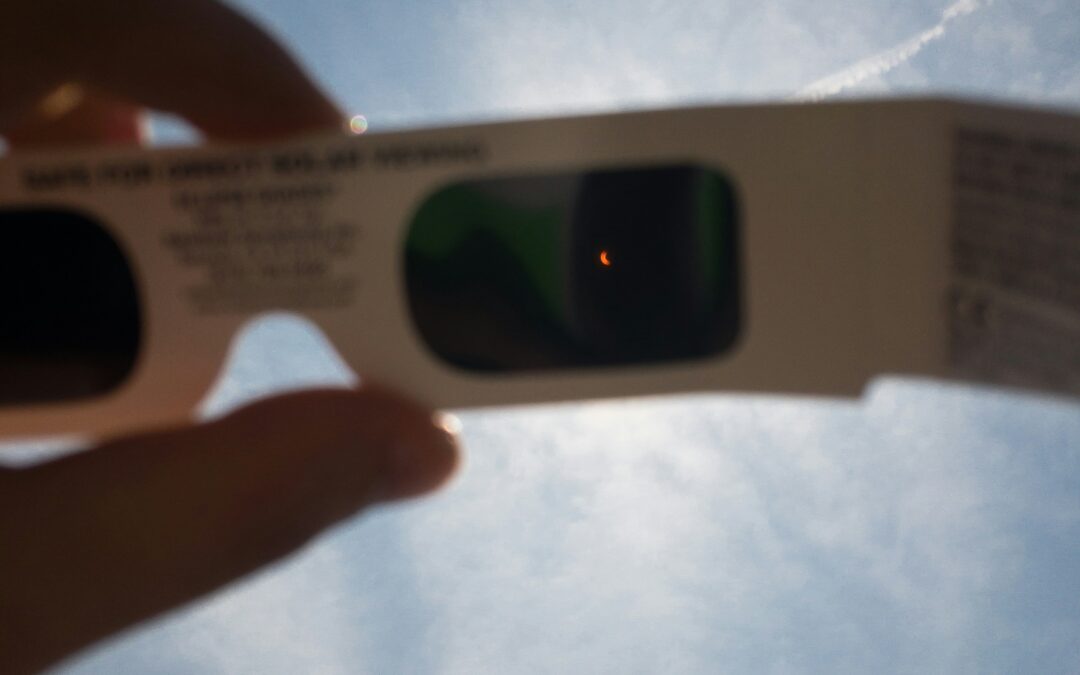
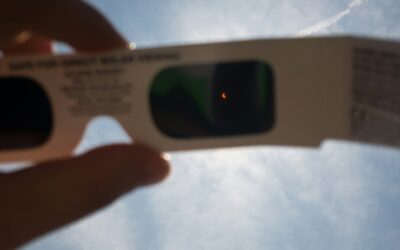
What To Expect During April’s Solar Eclipse
The Kitchen Pantry Scientist shares her tips on how to view the solar eclipse. Sky gazers are eagerly anticipating the upcoming solar eclipse on...

Candleberry on the Lakes Boutique Celebrates Spring
Visit a seasonal marketplace featuring handmade goods from local vendors. Candleberry on the Lakes Boutique has been around for over 40 years, but...

Petal Perfect
Unveiling sublime beauty of nature’s purple majesty. Judy Fulk cherishes Arneson Acres as her go-to haven for capturing the ideal photograph. Fulk,...
Popular Stories
Shop Local
La Bratique
If you’ve been blessed with curves and have a hard time managing your assets, schedule a private By-Appointment bra fitting with the Twin Cities' premier bra fit professionals. Our highly trained staff will hand select the best options for fit in Basics, Fashion and Sport bras. Brands such as Prima Donna, Fantasie, Freya, Elomi, Chantelle, Anita, Fit Fully Yours and Wacoal have all been carefully chosen for their quality fabrics, superior construction for D cups and up and beautiful detailing. Sizes 30D to 40K. Not only will you walk out with a killer silhouette, but the heaviness of your...
Noteworthy
French Toast With Minimal Effort
I love a good breakfast casserole that can be prepped ahead of time. This Brioche French Toast Casserole is absolutely perfect for an occasion like...
Feel the Rhythm With “Everything a Drum”
In this bouncy read aloud picture book from Minneapolis author Sarah Warren, a happy toddler makes everything in his home into a drum. “Ta-tum! Tum!...
From Yard to Garden
Making a house a home takes as much of an effort as making a yard a garden. The end product of your efforts is the pride of sharing an ideal place...
What To Expect During April’s Solar Eclipse
The Kitchen Pantry Scientist shares her tips on how to view the solar eclipse. Sky gazers are eagerly anticipating the upcoming solar eclipse on...
Events
Arbor Day Tree-Planting Celebration
Celebrate Arbor Day by learning how to plant a tree and then helping plant them at Centennial Lakes Park and the Edina Promenade. The event begins...
Edina Shark Tank 2024
On May 2, The Edina Chamber and Edina Public School District are thrilled to announce a chance to champion innovation in Edina and support the...
Green Tie Open Golf Tournament
Join us for a fun-filled day out on the course providing opportunities to connect and mingle with members of the Edina business community. The golf...
In This Issue

Candleberry on the Lakes Boutique Celebrates Spring
Visit a seasonal marketplace featuring handmade goods from local vendors. Candleberry on the Lakes Boutique has been around for over 40 years, but 2023 marked its newest chapter. “It started as a...

Welcome to the April 2024 Issue
It’s that time of year again where we indulge you, dear readers, in our semiannual homes edition. This issue explores the concepts of tradition and modernity. We highlight tradition with a look at a...

New Century Homes Project Preserves History
New program recognizes century-old homes. Edina’s Heritage Preservation Commission (HPC) introduced a new project aimed at historic appreciation, environmental awareness and celebration. It’s called...

Behind the Programs That Support Edina Students With Autism
Programs and resources help children and adults with autism find belonging, build skills and pursue their interests. If you visit a Unified class in an Edina school, you’ll see friends chatting or...

J.H. & Sons Is Made To Measure
New menswear shop blends two beloved stores. There’s a famous saying: The suit makes the man. But what about the rest of his wardrobe? For more than 100 years, famed haberdashery Hubert White was...